3 Key Pain Management Cost Trends in Workers’ Compensation Claims
Recent data from NCCI explores the composition of workers’ compensation costs related to pain management. We explore their findings, including some of the most common cost drivers.
March 23, 2026

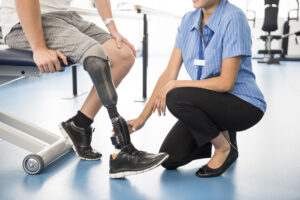
Following a work injury, an employee can experience varying degrees of pain, requiring treatments ranging from topical gels to major surgeries. The resulting costs in workers’ compensation claims can vary significantly, particularly with emerging therapies meant to replace the use of opioids.
“The industry has seen a sharp decline in the utilization of opioids, which is hugely beneficial for the long-term recovery of an injured worker,” said Jennifer Gallagher, Medical Manager at Safety National. “However, the decline in costs from these prescriptions is being offset by increasing costs in alternative treatments, like topical creams and gels. Private-label prescriptions and a lack of regulated pricing are contributing heavily to these costs, while physician dispensing can also increase prices. Additionally, compounded topicals that are made by combining multiple medications have both a drug cost and a compounding fee, which is generally not regulated and, in some circumstances, can be very costly on certain claims.”
We review the highlights from the National Council on Compensation Insurance (NCCI)’s recent report, Pain Management Interstate Variation.
1. For most states, pain management costs in workers’ compensation claims increased over the course of the study years, but at a lesser rate than total medical costs.
After analyzing data from 2023 to compare state-to-state costs on pain management per claim, the difference between the highest- and lowest-cost states was $5,025 per claim. Arkansas fell below the media at $1,402 per claim, while Louisiana rose above the media at $3,871 per claim.
Once varying types of medical conditions were considered and adjusted for, the range narrowed to $3,176 per claim. This adjustment changed the ranking of a few states, but most remained the same, indicating that factors beyond the mix of medical conditions contribute significantly to cost variance.
2 The largest contributors to pain management costs are major surgery, prescription drugs, and physical medicine, involving adjunct procedures such as injections and physical therapy.
Major surgery accounted for 34% of pain management costs, while prescription drugs and physical medicine each accounted for 14% in the medical services categories. Additionally, NCCI notes that costs for major surgery and physical medicine have increased over the last decade, with major surgery increasing at an average annual rate of 1.9% and physical medicine at 2.3%.
3. Strict physician-dispensing guidelines are helping to mitigate the costs of topical medications in certain states, but these prescriptions typically have associated high costs, which offset the decline in opioid costs.
NCCI found that, on average, opioids and topical medications account for 40% of drug costs per claim in the states surveyed. However, their cost contributions have changed significantly over the past 12 years. While the prescription and costs of opioids have decreased sharply, the costs associated with topical medications have risen, averaging between $10 and $630 depending on the state. NCCI points out that although topicals are prescribed less frequently than opioids once were, even a small increase in their usage can lead to substantial fluctuations in costs due to their wide range of pricing.