5 Best Practices for Managing Spinal Cord Injuries
An insurer’s medical management team can play a crucial role in ensuring an injured worker receives the best care available and regains their independence. We cover five key elements that make that journey possible.
January 13, 2023
According to 2022 data from the National Spinal Cord Injury Statistical Center at the University of Alabama at Birmingham (UAB), approximately 18,000 new spinal cord injuries (SCIs) are reported each year. Motor vehicle accidents and catastrophic falls — both of which can happen on the job — are the most common causes of SCIs in the United States.
Advancements in the medical field, like artificial intelligence, have decreased the amount of time it takes for many workers to recover from an SCI. Neural nets and robotic harnesses can help customize an injured worker’s experience, better mimicking the activities of day-to-day life. However, there are several important basic practices to follow to ensure an injured worker receives the best care and achieves independence in a timely manner.
“The ultimate goal for an injured worker who sustained an SCI is to maximize neuro-recovery and improve independence,” said Lisa Haug, Managing Director of Medical Management at Safety National. “Our role is to assist our insureds in providing or offering the best possible care for injured workers and offering insight into how to best coordinate care with centers of excellence for rehabilitation to maximize their recovery.”
The following are best practices to adhere to when managing spinal cord injuries:
1. Experienced Field Nurse
The number one best practice for managing SCI claims is ensuring a field nurse on the case, ideally, one experienced with managing catastrophic claims. It is imperative for the field nurse to be in continuous communication with the treating provider or assigned specialist.
2. Communication
Continual updates and coordination of care between all stakeholders, including the third-party administrator, field nurse, carrier, and insurer is critical. There should be collaboration between all parties to ensure the injured worker’s continuum of care is progressing appropriately, maximizing recovery in the process.
3. Centers of Excellence
It is essential that the injured worker is transferred to a center of excellence (CoE) to focus on their recovery. CoEs are multidisciplinary rehabilitation centers focusing on spinal cord injuries or traumatic brain injuries with an emphasis on cutting-edge research and innovation. These centers offer expertise and tools that may not be available for the injured worker regionally. Utilizing CoEs and vendor partners can help achieve the best possible outcome for the injured worker to maximize their recovery.
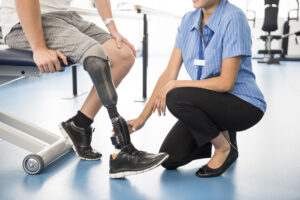
4. Promote Reintegration
The focus here should be on their abilities, not disabilities, working with all stakeholders to determine in what capacity the injured worker can return to work. This will aid in their physical and mental recovery and provide opportunities for community re-entry.
5. Mental Health
Addressing the psychological components associated with traumatic injuries is just as important as addressing the physical components. There is a high prevalence of post-injury depression in SCI patients, so further intervention requires analysis of all aspects of an injured worker’s well-being, including medical history, family support, and even their perception of pain.
Collaboration between all stakeholders is imperative to ensure a seamless transition to home, including ongoing medical support to improve their independence and overall well-being. Establishing this continued coordination of care can also help improve the likelihood of an injured worker returning to work and functioning as independently as possible.