Understanding the Severity and Treatment of Catastrophic Burn Injuries
Burn injuries remain one of the most devastating workplace exposures, often requiring prolonged care and accommodations. In this installment of our Catastrophic Injury Series, we explore how severe burns are assessed, treated, and managed to support optimal recovery outcomes.
March 9, 2026
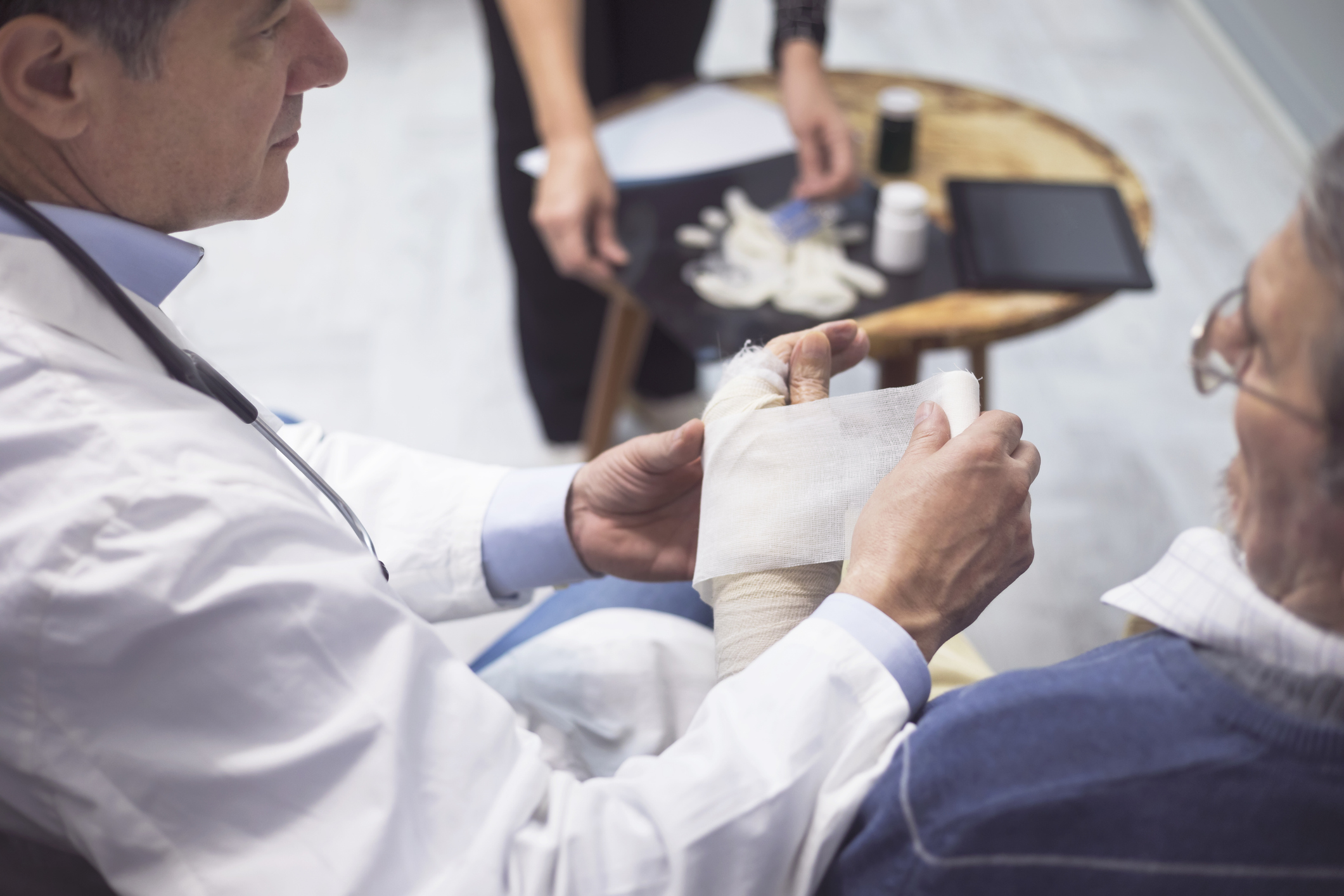
According to the National Institute of Health, there are approximately 450,000 to 500,000 burn injuries per year, with workplace injuries accounting for up to 45% of those incidents. While many of these burns can be minor, more serious catastrophic burns can be life-threatening, requiring ongoing medical care for an injured worker.
“Severe burns can cause rapid fluid loss, which can result in severe organ damage, infection, and shock in an injured worker,” said Lisa Strader, Senior Medical Manager at Safety National. “Fourth-degree burns that often cause these complications are typically a result of flames or chemicals. In patients with over 40% of their total body surface area burned, the risk for death is exceedingly high.”
To better understand the complexity of catastrophic burn injuries and their long-term implications, we address several key questions below.
What are the most common causes of this injury in the workplace?
Contact burn injuries in the workplace often involve grease fires, such as those from fryers, or contact with a hot object, such as a stove or tool. These can be classified as thermal burns because heat transfers very quickly, causing the burns to occur in seconds.
There are also chemical burns when individuals are working with substances such as industrial cleaners. Some catastrophic burns result from electrical contact among employees in professions that require contact with high voltage.
How is severity assessed in the early stages, and how does it shape the treatment plan?
Burn severity is classified by the Total Body Surface Area (TBSA) formula. The Rule of Nines is also utilized to estimate the TBSA affected. To calculate the TBSA, the injured worker’s body is divided into sections, which represent 9% each (or 9% total) for the TBSA. The calculation helps determine burn severity and guides treatment going forward.
Burns can range from first to fourth degree involvement. First-degree burns are relatively minor, whereas fourth-degree burns include all skin layers with the potential to include muscle, tendon, and bone injuries.
What does recovery and rehabilitation typically look like?
Severe burns often require specialized care and may need treatment at an American Burn Association-verified burn center. The centers have teams that have undergone extensive training and retain the resources to achieve the best possible outcomes.
Surgical treatments may include skin grafts, scar release procedures, and laser therapy for more involved burns. In addition, topical products are available, along with custom compression garments that assist with scar healing.
Patients may also need counseling and therapy. Individuals could have sustained life-altering events, disabilities or even disfigurements, and will require additional support not only physically, but emotionally as well.
What factors influence return-to-work outcomes?
Support on all fronts, including family structure, rehabilitation, and employer assistance, can aid an appropriate return to work. Consistent and open communication among the employer, adjuster, injured worker, and treating provider is valuable. The availability of modified hours or duties can often allow for a gradual return to work. There is also a possibility that an employee may require permanent accommodations or other adjustments.
Ultimately, it is a collaborative effort, and a case manager can be a valuable asset in facilitating the return-to-work process among the medical provider, injured worker, and claim adjuster.
What advancements in treatment, rehabilitation, or technology are improving outcomes?
Several advancements are being developed for burn treatment, including wound healing dressings, stem cell therapies, bioengineered skin substitutes, advanced pharmacological agents, and smart biomaterials. Advances will continue, as the global burn care market is projected to grow to over $4.2 billion by 2030.
Additionally, FDA-approved technologies, such as laser Doppler imaging and spray-on skin regeneration, are being used to more accurately assess burn depth and heal with reduced skin grafting needs. These advances are facilitating timely intervention and improving outcomes.